What is giant cell arteritis?
Giant cell arteritis (also arteritis temporalis) is a rheumatic autoimmune disease in which vascular inflammation occurs in the wall of the large blood vessels. Immune cells collect in the vessels and lead to chronic inflammation. It is not yet known why the disease occurs. Probably a hereditary predisposition in combination with specific external factors plays a role. Interestingly, giant cell arteritis is often accompanied by inflammation of the muscles and mucous membranes (polymyalgia rheumatica).
What are the typical symptoms?
A variety of non-specific symptoms, such as fever, weight loss, night sweats, muscle pain, headaches, pelvic and shoulder girdle pain, circulatory problems and visual problems, can be signs of the disease. Sometimes, a constant high level of inflammatory activity in the large blood vessels (aorta/abdominal aorta) can lead to destruction and instability of the vessel walls. This can later lead to a rupture of the vessel walls (aortic dissection/aneurysm).
Which examinations enable a diagnosis?
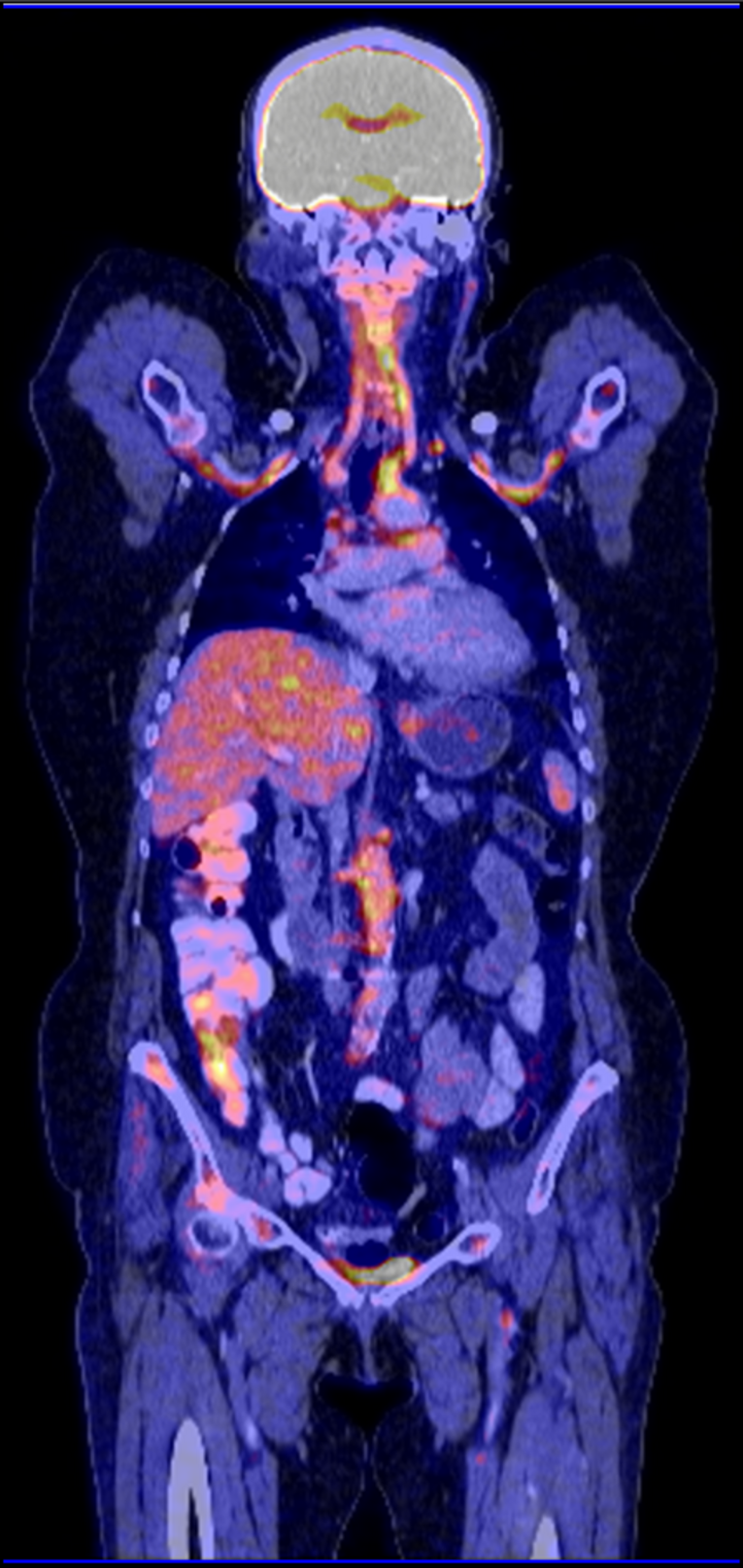
The diagnosis is made by the signs of inflammation in the blood and imaging procedures (ultrasound, magnetic resonance tomography and PET-CT) that make the vascular changes visible. A tissue examination of the temporal artery sometimes definitively confirms the diagnosis.
What can be done about the disease?
The most important component in treatment is a rapid start of long-term glucocorticoid (cortisone) therapy. A new therapy option is to block interleukin-6, an important pro-inflammatory messenger, so that the cortisone dose can be reduced.
Tips for everyday life
- If you suspect polymyalgia rheumatica and especially giant cell arteriitis, see a rheumatologist as an emergency
- The treatment of the disease is complex, so doctors from different specialities should be involved.
Consultation hour for Rheumatology and Immunology
Consultation hour
Zeiten
Monday - Thursday
07.30--15.30 h
Friday
07.30--12.30 h
Appointments only upon consultation
To schedule an initial appointment, please use the UKER's Emento Care-Guide app exclusively.
This allows us to record your request in a structured manner and prepare for it optimally.
Request an appointment online now
Please arrange check-up appointments by telephone with our outpatient team:
Phone: +49 9131 85-34742
Hinweis
Due to the high volume of patients, initial appointments can only be requested via the UKER's Emento Care-Guide app.
Request an appointment online now
Please arrange check-up appointments by telephone with our outpatient team:
Phone: +49 9131 85-34742
Downloads
Required documents
- Certificate of Insurance (health insurance card)
- Allocation
- Copies of the preliminary findings
- X-ray images
- Reports from previous hospitalizations
- in case of initial appointment, completed questionnaire (see documents)